Imagine your body has an army of fighters against cancer, but someone has deliberately reduced their power. That is essentially how the STUB1 protein works. Scientists at Harvard Medical School identified it as an important brake on the immune system’s anti-tumor response.
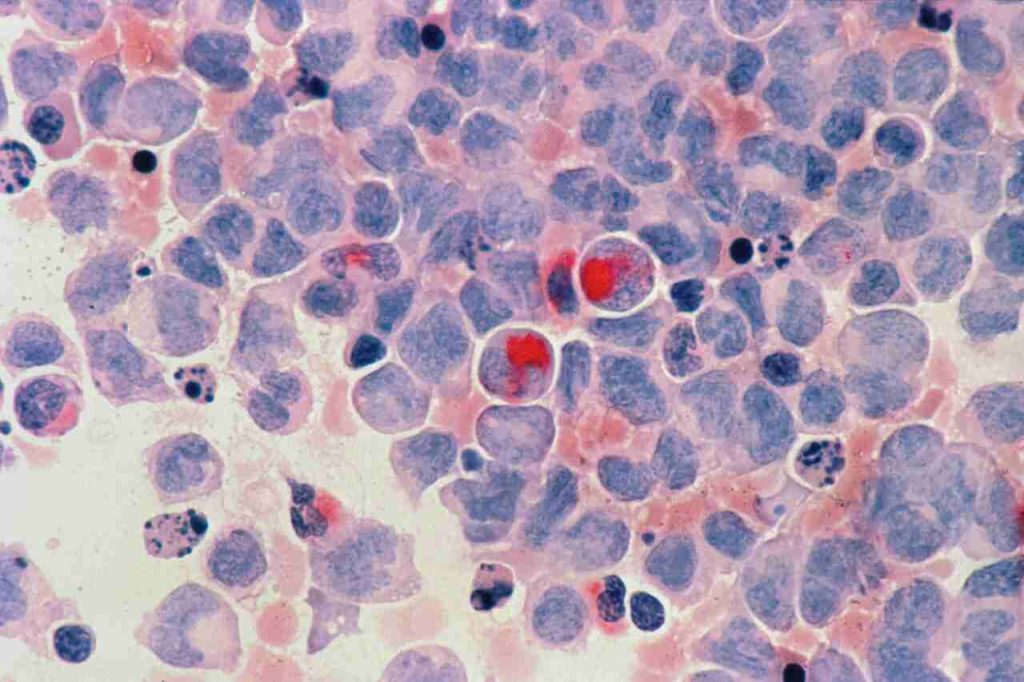
Your CD8+ T cells are the immune system’s elite units, tasked with seeking out and destroying tumor cells. They work like a special forces team that detects when something dangerous is happening in the body and moves in. But STUB1 gets in their way. It dampens their response to cytokine signals, the chemical messages that tell them it is time to attack. One of the most important molecules involved here is IL-27, which plays a key role in helping T cells launch a strong anti-tumor response.
In other words, a T cell needs the right signal to become fully activated and start attacking. STUB1 partially suppresses that signal.
An experiment involving nearly 900 genes revealed the main culprit
Researchers used CRISPR technology to examine nearly 900 genes. This is a tool that allows scientists to make highly precise changes to a cell’s genetic machinery and observe what happens when a specific gene is switched off. They were trying to answer one question: what exactly is holding T cells back from mounting an effective attack on tumors?
Out of all the genes they tested, one stood out: STUB1. When scientists removed it from CD8+ T cells, those cells became markedly better at fighting tumors. Mice with these modified T cells developed slower-growing tumors and lived longer.
That matters because this was not just a minor lab effect. It means that once this “brake” was removed, immune cells performed visibly better in a living organism.
“Even though cancer immunotherapies have transformed the way we treat cancer, it’s important that we find new ways to extend these lifesaving and life-changing benefits to more people,” said lead author Martin LaFleur.
Two proteins switch off the T cells’ combat gear
STUB1 does not act alone. It works together with another protein called CHIC2. When the two join forces, they remove key receptors from the surface of T cells.
To picture this more easily, receptors are like tiny “antennas” on the surface of a cell. Through them, the cell receives instructions from its surroundings. If those antennas are gone, the cell is still there, but it can no longer properly understand what is happening around it.
The result is that T cells stop properly sensing signals from cytokines, the molecules meant to activate them. You can think of cytokines as chemical messages passed between immune cells. One cell sends the signal, another receives it and acts accordingly. But if the receptor is missing, the message never gets through. It is a bit like having your phone switched off and not realizing someone is calling for help.
Human cells responded similarly to mouse cells
Although most of the experiments were carried out in mice, the scientists also tested their findings in human T cells. When they removed STUB1 or CHIC2, cytokine receptor levels increased, just as they had seen in mice.
This is important because the effect did not appear only in mice. Scientists saw it in human T cells as well, suggesting that this mechanism may not be limited to an animal model.
On top of that, previous research had already shown that IL-27 is associated with a stronger T-cell response and more effective immunotherapy in human patients. That suggests that blocking STUB1 could also strengthen IL-27 signaling in humans.
Two possible paths toward a new cancer treatment
Scientists see two ways to turn this discovery into a real treatment. The first is to develop a drug that blocks STUB1, and they are already working on that. The second is to modify T cells so that they do not have STUB1 at all.
The first option would work more like a conventional treatment, meaning the patient would receive a compound that suppresses this brake. The second route is technically more ambitious, but also highly intriguing. Scientists would take a patient’s T cells, modify them outside the body, and then return them stronger and better prepared for battle.
This second strategy looks especially promising. STUB1 is found in multiple parts of the body, so selectively removing it only from T cells could strengthen their function while also minimizing the risk of potential toxicities that might arise if the protein were suppressed throughout the entire body.
Put simply, if you switch off the brake only where you actually need to, there is less chance of disrupting the function of other healthy cells.
Current immunotherapies do not help every patient
This discovery comes at a time when medicine truly needs it. Current cancer immunotherapies work in fewer than half of the patients who receive them.
That is why scientists are looking for additional mechanisms they can target. Tumors often do not overpower the immune system through sheer force. Instead, they exhaust it, confuse it, or slow it down.
Blocking STUB1 could therefore work on two fronts at once. On one hand, it could strengthen the anti-tumor response of T cells. On the other, it could make tumors themselves more vulnerable to attack.
STUB1 could also be combined with existing treatment
Scientists believe STUB1 inhibition could work as a standalone treatment, but also in combination with existing therapies. Because STUB1 affects the early stages of T-cell activation, it could pair well with treatments that act later in the immune response.
In oncology, a single miracle drug is rarely what wins the fight. More often, success comes from a well-designed combination of several approaches. One intervention gets immune cells ready to attack, another helps them endure, and another weakens the tumor itself.
“We anticipate that STUB1 inhibition could be effective either as a monotherapy or in combination with existing cancer treatments. Given that STUB1 influences early T-cell priming, it may serve as an effective combination therapy with other treatments that act later in the T-cell response,” LaFleur explained.
The researchers also stress that further studies will be needed to fully understand how effective and safe STUB1 inhibition would be in humans. Even so, it is already clear that their discovery offers a new perspective on how the immune system fights cancer and how we may be able to help it fight more effectively in the future.